Achilles Tendonitis: Symptoms, Causes, Risks and Podiatry Treatments
Did you know that at some point in their training, Achilles tendinitis affects up to 30% of runners? As someone potentially experiencing this condition, you’d notice morning stiffness, pain, swelling, and difficulties in activities like walking, which hint at underlying inflammation or scar tissue formation.
Factors such as overuse and inappropriate footwear often contribute, with increased risk emerging from intensified training regimens and pre-existing health issues. Podiatric treatments, ranging from custom orthotics to targeted exercises, offer relief. However, advanced interventions, like shockwave therapy, might be integral to enhanced recovery.
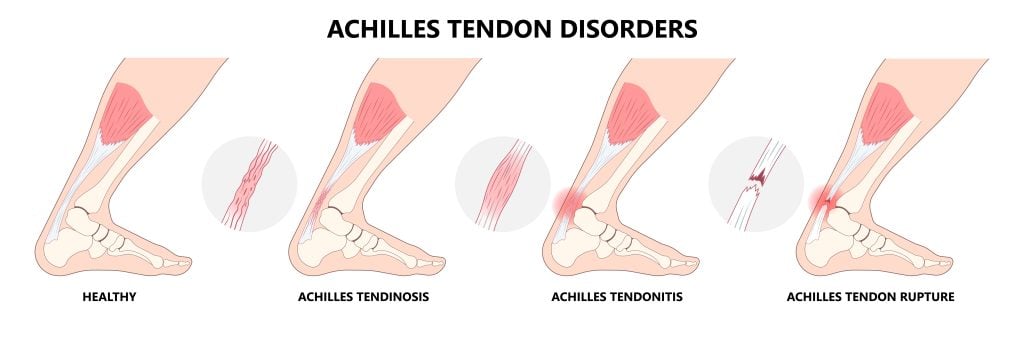
Symptoms of Achilles Tendon Pain
If you’re experiencing Achilles tendon pain, you might notice morning stiffness and difficulty when walking.
A palpable lump along the tendon could indicate localised inflammation or a partial tear.
Address these symptoms promptly to prevent further damage and facilitate recovery through targeted therapies like custom orthotic support and physical therapy exercises.
Tendon Pain
Although often gradual in onset, Achilles tendon pain is characterised by distinct symptoms that can greatly impact your daily activities.
You’ll likely experience swelling, tenderness, and a peculiar stiffness in the back of your heel. These symptoms could indicate anything from an acute tendon injury to chronic Achilles tendinopathy.
Timely tendon treatment helps prevent debilitating complications like tendon rupture. Treating Achilles tendon pain involves addressing these symptoms with targeted therapies, such as specific exercises and therapies for Achilles tendonitis.
Morning Stiffness
When you encounter morning stiffness in the Achilles tendon, it indicates stress or inflammation affecting your musculoskeletal system.
This stiffness often greets you with increased pain in the heel area, making those first steps out of bed challenging. Achilles tendonitis is characterised by this discomfort, which you should not ignore.
Recognising that inflammatory processes or even tendon degeneration could cause this symptom is crucial.
Noticable Lump
When recognising symptoms of Achilles tendon pain, some may notice a detectable lump in the tendon area, indicating potential issues such as inflammation or degeneration. This discernible lump is often due to scar tissue buildup, damaged tendons, or calcification, which may lead to further discomfort and pain. An anatomical examination can help confirm the presence of this mass, distinguishing it among various stages of Achilles tendinitis.
When you detect these changes, it’s essential to seek the expertise of a podiatrist. They can assess whether inflammation or degeneration is predominant in your condition, guiding treatment pathways effectively. Tactile exploration of the area might reveal tenderness or a firmer consistency, indicative of disease severity.
Walking Difficulties
Not only can a noticeable lump signal potential issues with your Achilles tendon, but it may also forewarn of walking difficulties stemming from tendon pain. Suffering from Achilles tendinitis often translates to heel pain and significant walking limitations. You might find yourself struggling with gait abnormalities that make every step painful. Your ability to bear weight on the affected foot decreases, complicating tasks that should be simple.
Morning stiffness adds another layer of complexity, posing challenges in taking those essential first steps of the day. But don’t let this deter your pursuit of freedom; recognising early symptoms is crucial in regaining mobility. An effective management plan, including podiatric interventions, can address and alleviate this discomfort.
To manage these achilles symptoms effectively, early diagnosis and a patient-focused treatment approach are essential. This may include interventions aimed at reducing inflammation & pain, improving tendon flexibility, and restoring normal function to support the patient’s desire for an active lifestyle.
Achilles Tendinitis Common Causes
Understanding the root causes of Achilles tendinitis in sports medicine and podiatry is essential for effective tendon treatment and prevention strategies:
- Achilles tendinitis often stems from overuse, where repetitive strain and increased training frequency without proper rest become detrimental to the tendon.
- Sports-related activities, like running and jumping, place continuous stress on the Achilles, making it susceptible to damage. As an athlete or active individual, you're likely pushing your limits.
- However, remember that incorrect foot biomechanics, such as flat feet or improper footwear, can exacerbate the strain on your tendons.
- Moreover, muscle imbalances play a significant role. The risk of developing tendinitis increases when calf muscles are too tight or your lower leg muscles aren't properly coordinated.
- Insufficient warm-up routines and insufficient recovery time between workouts only exacerbate these problems by preventing the tendon from adequately repairing itself before stress.
Remember, Achilles tendinitis isn’t unavoidable. Addressing improper training progression and focusing on correct stretching techniques can greatly reduce your risk. Embrace the freedom that comes with a healthy and responsive body by taking proactive steps towards correct biomechanics and balanced, mindful achilles exercise routines.
Achilles Tendinopathy Risk Factors
When considering Achilles tendinopathy risk factors, you should focus on high-impact sports and tight calf muscles, as they can greatly contribute to tendon strain and pain.
Incorrect footwear may exacerbate this achilles pain by failing to provide adequate support or cushioning.
Additionally, the intensity of your training and demographic factors, such as age and gender, can increase your susceptibility to these pain issues.
High Impact Sports
High-impact sports increase the risk of Achilles tendinopathy due to repetitive stress and mechanical overload on the tendon. They engage in activities like basketball, soccer, and running, which subject your insertional and non-insertional Achilles to substantial force, potentially leading to Achilles tendinosis.
These sports’ stop-start movements and high-intensity bursts often cause micro-tears, increasing the likelihood of detaching the Achilles tendon if not managed properly.
Tight Calf Muscles
Tight calf muscles greatly increase the risk of Achilles tendinopathy by placing excessive strain on the Achilles tendon. When your calf muscles are inflexible, they alter biomechanics during activities such as running and jumping.
This inflexibility reduces ankle joint mobility, forcing the Achilles tendon to bear more load, thereby predisposing you to Achilles tendinitis. Fortunately, surgical treatment isn’t the first step.
Address tight calf muscles through targeted stretching and flexibility exercises to effectively prevent and manage Achilles tendinopathy.
Poor Footwear
Improper footwear’s role in Achilles tendinopathy is significant, as wearing unsupportive shoes can increase stress on the Achilles tendon. Shoes lacking arch support or cushioning compromise the tendon’s stability, causing undue strain and increasing the risk of injury.
Inadequate shock absorption, often found in casual or high-heeled shoes, magnifies this stress by altering your natural gait. Consequently, the Achilles tendon must exert more effort to accommodate these changes, predisposing it to microtrauma.
Tight or ill-fitting shoes can distort your biomechanics, placing additional pressure on the tendon. Every step in such footwear can compound the risk of developing Achilles tendinopathy. To protect your Achilles tendon and retain freedom of movement, support the foot with shoes that enhance anatomical function.
Training Intensity
The intensity of your training regimen is a critical determinant in developing Achilles tendinopathy, where sudden escalation can overstress this robust yet vulnerable tendon.
Running, jumping, and stop-start sports inherently subject the Achilles tendon to significant forces. Rapid intensification of these exercises without adequate progression increases the risk of micro-injuries and subsequent degenerative changes.
Demographics
Analysing demographics and risk factors for Achilles tendinopathy reveals critical insights into its prevalence and prevention.
For starters, if you’re a man over 30, you’re in a higher risk category, especially if athletic activities or higher body weight are part of your lifestyle.
The anatomical structure of your Achilles tendon, combined with repetitive strain, makes you more vulnerable.
Chronic Health Conditions
Traversing the intersection of chronic health conditions and tendon health reveals crucial insights into risk factors for Achilles tendinopathy.
If you’ve got chronic diseases like diabetes, hypertension, or obesity, you face increased chances of developing this condition. Due to impaired circulation and metabolic imbalances, diabetes affects your tendon’s structural integrity, making it more susceptible to degeneration and slower healing.
Hypertension compounds the issue by potentially diminishing tendon resilience. These altered physiological states invite overuse injuries, with the Achilles tendon particularly vulnerable.
Understanding these risk factors empowers individuals to make informed decisions about their physical activities and lifestyle choices, thereby reducing the likelihood of developing Achilles tendinitis injuries and preserving their freedom to engage in desired sports and activities.
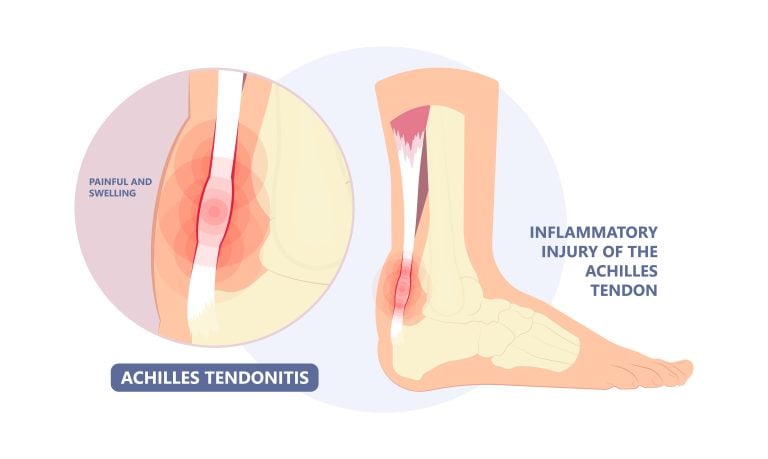
Achilles Health Tendon Treatment
Bellevue Podiatry offers specialised treatment for Achilles tendinitis that not only alleviates symptoms but also holistically manages and treats the condition for long-term recovery. We offer personalised care to reduce pain, inflammation and strengthen the Achilles tendon, addressing pain, swelling, and limited ankle dorsiflexion.
Your journey to recovery involves a carefully crafted treatment plan. Imagine the freedom you’ll feel as these steps guide you back to health:
- Custom Orthotic Therapy: Tailored insoles help correct foot biomechanics, providing the support needed to prevent undue tension on the tendon.
- Shockwave Therapy: This non-invasive procedure stimulates the body's intrinsic repair mechanisms, hastening recovery and reducing pain.
- Targeted Exercises: Specific stretches and strengthening regimens designed by your podiatrist bolster the tendon and surrounding muscles, enhancing flexibility and endurance.
- Rehabilitation Programmes: Safely resume your beloved sports with confidence, thanks to all-encompassing rehabilitation tailored to restore full function.
These treatments are patient-focused, aiming to enable individuals to regain freedom of movement efficiently and effectively.
Preventive Tendon Treatment Health Measures
Incorporating preventive health measures is essential to sustain the benefits of Achilles Health Podiatry’s treatment and promote long-term tendon resilience:
- Start by gradually progressing your exercise routine to avoid sudden stress on the Achilles tendon. Moving slowly in activities helps your tendon acclimatise to new demands, reducing injury risk.
- Opt for proper footwear that offers adequate arch support and cushioning to distribute pressure evenly across your foot structure, which is important for preventing undue strain on your tendon.
- Incorporate daily stretching to maintain flexibility in the gastrocnemius and soleus muscles, easing tension on the tendon.
- A structured regimen of strengthening exercises aids proprioception and enhances muscle-tendon unit durability.
- Pay attention to your body's signals; recognising early overuse or strain allows timely adjustment to your activity levels.
- Regular podiatrist consultations can provide tailored advice aligning with your unique biomechanics. They can assess your foot architecture and recommend personalized interventions.
Maintain an active lifestyle with intentional care—letting you enjoy greater freedom and fewer restrictions. Adhering to these preventive strategies fortifies your Achilles tendon, paving the way for sustained mobility and enhanced podiatric health.
When To Seek Professional Help
Experiencing persistent pain or stiffness in your Achilles tendon can be indicative of a condition that requires professional evaluation. If home remedies haven’t resolved your discomfort, it may be time to consult a podiatrist.
Persistent symptoms such as swelling and difficulty with everyday activities, like walking or standing on your toes, deserve careful assessment. You shouldn’t ignore noticeable lumps in the tendon area as they could signal a more significant problem.
Professional help becomes pivotal in several scenarios:
- Difficulty walking or standing on toes persists: These challenges can hinder your daily life and stall recovery.
- Noticeable lumps in the tendon area: These could indicate overgrowth or serious tendon issues that need expert attention.
- Ongoing discomfort during physical activities: Consistent pain amidst activity can worsen without proper intervention.
- Popping sound with severe tears: This alarming sound often signals a severe issue needing immediate care.
A podiatrist will assess your condition and recommend a treatment plan tailored to your needs. Utilising modern therapies and personalised exercises, professional intervention will alleviate discomfort and support tendon healing. Prompt action can help preserve your mobility, allowing you the freedom to engage in activities you enjoy.
Conclusion
Achilles tendinitis, akin to a persistent thorn in one’s heel, arises mainly from overuse, improper biomechanics, and inadequate footwear.
Effective management through podiatry treatments, including custom orthotic therapy, shockwave therapy, targeted exercises, and foot mobilisation techniques, is vital for alleviating symptoms and promoting recovery.
An emphasis on preventive measures, such as appropriate footwear and biomechanical correction, is necessary to reduce the risk of recurrence and ensure long-term tendon health.
