Diabetic Feet Problems: Symptoms, Podiatry Treatment, and Care
Diabetic feet problems often manifest through a variety of symptoms, such as changes in skin colour and temperature, persistent swelling, and slow-healing sores, all of which can lead to severe complications if left untreated.
Podiatrists are essential in the early detection and management of these issues, offering tailored treatment plans and preventive care strategies. From medication and wound care to surgical interventions, the scope of podiatry care is extensive and crucial.
Understanding the importance of daily foot care routines and preventive measures can greatly reduce the risk of complications.
Symptoms of Diabetic Feet Problems
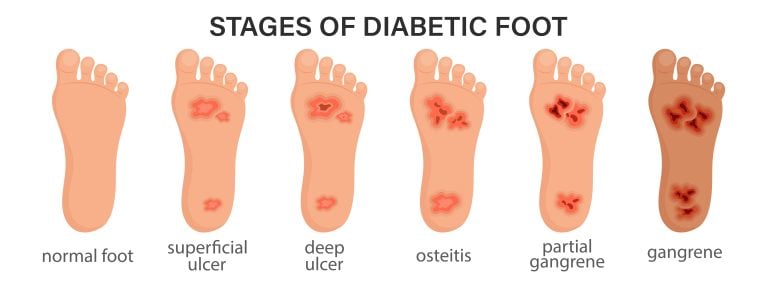
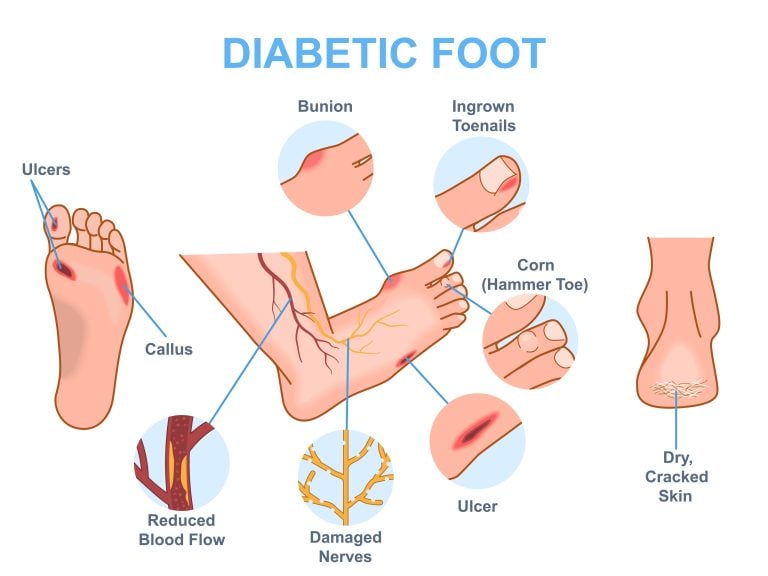
Symptoms of diabetic feet problems can include noticeable changes in skin colour and temperature, persistent swelling, and slow-healing sores. These symptoms frequently indicate underlying issues, such as diabetic neuropathy or peripheral artery disease, both of which are common complications of diabetes affecting the feet:
Neuropathy
Diabetic neuropathy, characterised by numbness, tingling, or burning sensations, is a result of nerve damage and can lead to unnoticed injuries due to reduced sensation.
Feet Ulcers
Another significant concern is the development of diabetic foot ulcers, which are open sores that fail to heal properly due to impaired blood flow and compromised immune response. Such ulcers require prompt and effective diabetic foot ulcer treatment to prevent severe complications, including infections that can lead to deformities or even amputations.
General Foot Health
Additionally, common foot issues like blisters, corns, calluses, and fungal infections can exacerbate the risk of more serious conditions in diabetic feet.
Recognising and addressing these symptoms early is critical for maintaining foot health and preventing further complications related to diabetes and feet.
Role of Podiatrists
Given the range of symptoms associated with diabetic feet problems, the role of podiatrists becomes essential in managing these complex issues.
Podiatrists are specialised healthcare professionals adept at diagnosing and treating foot conditions, particularly in individuals with diabetes.
Their expertise includes comprehensive assessments of circulation, sensation, and foot structure, which are critical in preventing serious complications such as ulcers and infections.
Podiatrists conduct regular foot examinations to detect early signs of neuropathy, ischemia, and other foot-related issues common to diabetic patients.
By identifying these symptoms early, podiatrists can formulate customised care plans tailored to each patient’s specific needs.

These plans may include recommendations for appropriate footwear, daily foot care routines, and strategies to enhance blood flow. Moreover, podiatrists play a pivotal role in educating patients on maintaining excellent foot health. They provide guidance on daily inspections, proper hygiene, and the importance of glycemic control to mitigate the risk of foot complications.
Regular visits to a podiatrist ensure continuous monitoring and timely intervention, thereby reducing the likelihood of severe outcomes such as amputations. This proactive approach underscores the important contribution of podiatrists to the thorough management of diabetic feet problems.
Effective Treatment Options
To effectively manage diabetic feet problems, a holistic treatment strategy encompassing medication, wound care, debridement, and surgical interventions is vital:
Infection Medications & Foot Topical Agents
Diabetic foot ulcers often require the prescription of medications to treat infections. We can use systemic antibiotics to fight bacterial infections, and topical agents to treat localised areas.
Foot Wound Care
Wound care is a critical component, involving regular cleaning, dressing, and monitoring to guarantee proper healing. Advanced wound care techniques, such as the use of growth factors and bioengineered tissue substitutes, can accelerate recovery and reduce the risk of complications.
Feet Debridement
Podiatrists perform debridement, the removal of dead or infected tissue, as a pivotal procedure to promote the formation of healthy tissue and prevent further infection. Depending on the severity of the wound, podiatrists can perform this surgically or through less invasive methods.
Foot Surgicial Interventions
In cases where conservative treatments are insufficient, surgical interventions may be necessary. These can range from minor procedures, such as the removal of calluses or necrotic tissue, to more extensive surgeries aimed at correcting deformities or improving blood flow.
Footwear / Shoes Modifications
Custom orthotic devices and footwear modifications are also paramount in alleviating pressure points and preventing further damage. Regular podiatric assessments ensure early detection and timely management, substantially improving patient outcomes.
Daily Foot Care Tips
Daily foot care is essential for individuals with diabetes to prevent complications such as ulcers, infections, and neuropathy-induced injuries. Implementing a daily routine is vital for maintaining foot health and minimising the risk of serious conditions:
Begin by inspecting your feet daily for any signs of cuts, blisters, redness, or swelling.
Use a mirror to examine the soles of the feet, or seek help if necessary.

To prevent fungal infections, practice proper hygiene by washing your feet daily with lukewarm water and mild soap, and make sure to thoroughly dry them, especially between the toes.
Moisturising the feet and avoiding the areas between the toes helps prevent dry, cracked skin, which can lead to infections.

To prevent ingrown toenails, trim nails straight across and file the edges.

Wearing well-fitting, comfortable shoes with adequate support and a wide toe box is crucial to avoid pressure points and friction that can cause ulcers and ingrown toenails.

Promptly seek medical attention for any non-healing sores, changes in skin colour or temperature, or slow-healing wounds. Adhering to a healthcare provider’s recommendations on blood sugar management, nutrition, and exercise is indispensable for optimal foot health. We strongly recommend regular podiatric evaluations to promptly address any emerging issues.
Foot Health Assessments
Early recognition of potentially serious foot health issues gives you the best chance of curing them before they become a serious problem – the earlier you find them, the better. You should book in and see an experienced Podiatrist if you have diabetes because:
- Diabetes can lead to nerve damage and loss of sensation
- You can develop foot deformities
- There can be changes to your arteries leading to decreased blood supply
At Bellevue Podiatry we have advanced assessment equipment to determine if you have had any of these changes. Our podiatrists are experienced in the assessment, management, education and prevention of diabetes related foot pathologies.
A diabetes assessment includes:
- A general health questionnaire
- Diabetes control and effects on your overall health
- Vascular supply including a doppler assessment, ankle brachial index and toe pressure reading, giving us a better understanding of the blood supply to your feet
- Protective sensation with a monofilament and vibration fork
- Joint range of movement and deformities
- Footwear assessment
- Dermatological assessment
From this assessment we will be able to determine:
- Ability to feel (for example – will you be able to feel a blister developing on your foot?)
- Blood flow (if you have a cut on your foot is there enough blood there to help it heal?)
- Any obvious changes to your foot structure (will a bunion rub on shoes?)
With this information we can provide you tips and strategies to prevent complications such as blisters, ulcers or wounds, joint deformities, infections and amputation – a very prudent investment for the cost and time of a 30 minute consultation.
When To Seek Professional Help
You should seek professional help when you notice any changes in your feet, such as color alterations, temperature shifts, or persistent swelling. These could indicate underlying issues that need prompt attention. Slow-healing sores or symptoms of diabetic neuropathy like numbness, tingling, or burning sensations also warrant a consultation with a podiatrist.

Ignoring these signs due to a feeling of necessity can lead to serious complications, including infections or even amputations.
Podiatrists are crucial allies in your diabetes management strategy. They provide early detection through thorough examinations and tailor treatment plans to your specific needs. With their expertise, they can address foot ulcers, infections, and any emerging deformities efficiently.
By incorporating regular visits to a podiatrist into your health routine, you’re not just reacting to issues— you’re proactively safeguarding your independence and wellbeing.
Taking control by seeking timely professional intervention empowers you to maintain active participation in your care. By engaging with your podiatrist, you not only receive immediate treatment but also benefit from preventive measures that keep further complications at bay.
Your proactive steps are imperative for ensuring continuous freedom and mobility.
Conclusion
In the domain of diabetic feet care, vigilant attention to symptoms is paramount. Do not overlook symptoms such as altered skin colour and temperature, persistent swelling, and slow-healing sores. Podiatrists, with their clinical expertise, act as guardians of your foot health. To effectively address these symptoms, they use advanced treatment modalities and individualised care plans.
Through the precise implementation of wound care, surgical interventions, and custom orthotics, alongside daily foot care practices, the path to preventing complications and fostering excellent foot health becomes clearer and more attainable.
Know your risk – a short 30 minute consult could save your feet. Book in today to see one of our experienced Podiatrists, call us on (03) 4237 7165 or book online.
Diabetic Foot
Understand what diabetes means for your feet and make sure you know the steps to protect your foot health long term. Learn how to avoid unnecessary foot health complications to keep your feet and toes healthy for life.

