That persistent, throbbing discomfort around your first metatarsophalangeal joint is a clear signal that something structural is changing, and it warrants proper assessment rather than simply tolerating it. Bunions, or hallux valgus deformities, do not self-correct, but surgical intervention is far from the only pathway to meaningful relief and preserved function.
With the right conservative management — including orthotics, targeted footwear modifications, and guided physical therapy — it is entirely possible to reduce pain, slow the progression of the deformity, and maintain your quality of life. The key is acting before the joint deteriorates further, as early intervention consistently produces the best outcomes in non-surgical bunion care.
In This Article
- Custom orthotics redistribute pressure away from the first MTP joint, correcting faulty foot mechanics and reducing pain without surgery.
- Wide toe box footwear, gel bunion shields, and metatarsal padding reduce compression and friction on the affected joint.
- Early intervention produces measurably better outcomes and preserves more conservative treatment options before structural joint damage occurs.
- Bunion mobilisation therapy combined with orthotics and footwear changes lowers daily pain and slows deformity progression effectively.
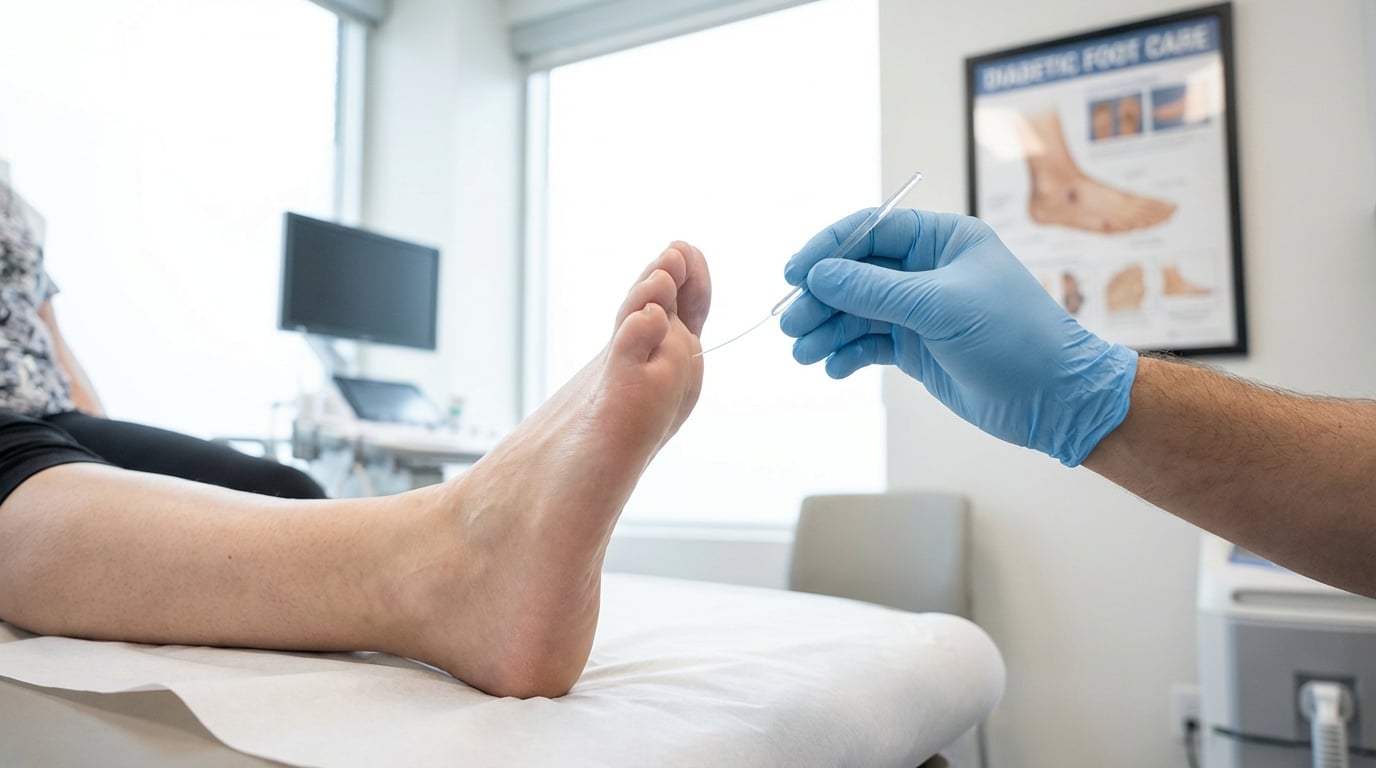
- Thorough bunion assessment at Bellevue Podiatry in Rosanna identifies underlying causes and establishes a clear conservative treatment plan.
Why Bunions Cause Daily, Throbbing Shoe Pain
When a bunion forms, it forces the first metatarsophalangeal (MTP) joint out of anatomical alignment — and that structural deviation is the primary driver of your daily discomfort. The bony prominence rubs persistently against the inner surface of your shoe, inflaming the surrounding soft tissue and bursal sac with every step.
Every step drives that bony prominence deeper into your shoe — inflammation isn’t incidental, it’s structural.
Standard footwear compresses the forefoot, placing direct pressure on the deviated joint and intensifying localised irritation throughout the day.
For many patients presenting with bunion pain at our Melbourne clinic, unsupported foot mechanics are accelerating the condition just as much as the bunion itself.
Effective management requires addressing load distribution across the entire foot, not just the site of pain. This is where custom foot orthotics serve as the most clinically effective conservative treatment option available.
Understanding the Root Cause of Your Bunion Deformity
Before you can effectively address your bunion pain, you need to understand what’s actually driving the deformity in the first place.
Genetics plays a significant role — if your mother or grandmother had bunions, your inherited foot structure and joint mechanics likely put you at higher risk, regardless of your shoe choices.
However, years of wearing narrow, constrictive footwear combined with underlying flat feet or collapsed arches can dramatically accelerate that genetic predisposition, forcing your big toe joint into a progressively worsening misalignment.
The Impact of Genetics vs. Narrow Footwear
Narrow toe boxes, elevated heels, and rigid work shoes place sustained mechanical force on the first metatarsophalangeal joint, gradually driving the big toe into an adducted position. While genetics determine your baseline joint structure and ligamentous laxity, footwear choices significantly influence whether that predisposition progresses into a symptomatic bunion deformity.
If you’re seeking a bunion assessment, understanding this distinction is clinically important — because it confirms that modifiable factors are within your control. Selecting appropriate footwear for bunion pain reduces abnormal joint loading, slows angular progression, and meaningfully decreases daily discomfort without requiring immediate surgical intervention.
The Hidden Role of Flat Feet and Poor Arch Support
Although bunion deformity is frequently attributed to footwear alone, flat feet and a collapsed arch structure contribute equally to how rapidly the condition develops and progresses.
When the arch fails to maintain its structural integrity, the forefoot absorbs abnormal rotational forces, accelerating metatarsophalangeal joint deviation.
Poor arch mechanics directly drive bunion progression through several biomechanical pathways:
& Collapsed arches redistribute body weight excessively toward the first metatarsophalangeal joint
& Excessive pronation forces the hallux to angle medially with every weight-bearing step
& Weakened arch support increases plantar pressure across the entire forefoot
& Unaddressed pes planus accelerates articular cartilage wear within the joint itself
Custom foot orthotics correct this mechanical imbalance at its source, reducing the abnormal forces that drive joint deformity over time.
As part of a structured conservative bunion management programme, our patients at Bellevue Podiatry benefit from tailored arch support designed to deliver measurable, long-term symptomatic relief without surgical intervention.
Can You Fix a Bunion Without Invasive Surgery?
Non-surgical bunion treatment focuses on managing pain, slowing progression, and improving your overall quality of life. At Bellevue Podiatry, we regularly help patients avoid surgery through a structured combination of custom orthotics, targeted footwear guidance, and evidence-based conservative care.
Custom orthotics work by redistributing pressure away from the affected first metatarsophalangeal joint, correcting the underlying biomechanical imbalances that drive symptom progression. For many patients, this approach delivers meaningful, lasting relief without the need for surgical intervention.
Advanced Non-Surgical Bunion Treatment at Bellevue Podiatry
At Bellevue Podiatry, we offer advanced, clinically proven non-surgical treatments that address the root cause of your bunion pain rather than masking it.
Our custom orthotics are precision-engineered to correct the faulty foot mechanics driving your bunion’s progression, redistributing pressure away from the inflamed joint with every step you take. Paired with targeted footwear modifications and protective padding, this all-encompassing approach gives you genuine, lasting relief without a single incision.
Custom Orthotics to Realign Your Foot Mechanics
Custom orthotics are one of the most clinically effective conservative interventions when bunion pain persists despite standard management. Unlike generic insoles, prescription orthotic devices are biomechanically engineered to your specific foot structure, addressing the underlying mechanical dysfunction rather than simply masking symptoms.
These devices support non-surgical management by delivering four key functions:
- Redistributing plantar pressure away from the painful first metatarsophalangeal joint
- Correcting abnormal foot pronation that accelerates bunion progression
- Complementing bunion padding and splints for more thorough joint offloading
- Stabilising your gait pattern to reduce cumulative inflammatory stress on the joint
When paired with appropriate footwear modifications, custom orthotics create a consistent mechanical environment that genuinely slows deformity progression and supports comfortable, functional movement over the long term.
Footwear Modifications and Protective Padding
Alongside custom orthotics, footwear modifications and protective padding form a critical second layer of conservative bunion management. At Bellevue Podiatry, your treatment plan directly addresses how your footwear interacts with the first metatarsophalangeal joint.
| Modification | Benefit |
|---|---|
| Wide toe box footwear | Reduces lateral joint compression |
| Gel bunion shields | Relieves shoe friction on the toe |
| Stretching tight shoe uppers | Creates immediate pressure relief |
| Metatarsal padding | Redistributes forefoot load |
| Bunion foot mobilisation therapy | Restores joint movement and reduces stiffness |
Each of these interventions serves a specific mechanical purpose and is most effective when applied in combination. When footwear stops compressing the joint and padding absorbs friction, daily pain levels typically reduce in a clinically meaningful way. This allows you to maintain mobility and function without progressing towards surgical consideration.
Stop Ignoring the Pain and Protect Your Mobility
Many women make the mistake of pushing through bunion pain, assuming it will resolve without intervention — but untreated hallux valgus consistently accelerates joint deterioration and compromises long-term mobility.
Untreated bunion pain doesn’t resolve on its own — it silently accelerates joint deterioration and steals your long-term mobility.
At Bellevue Podiatry, we regularly see patients who’ve delayed care, often presenting with significantly more advanced deformity than necessary.
Early hallux valgus treatment produces measurably better clinical outcomes.
The longer the deformity progresses without biomechanical correction, the more limited your conservative treatment options become.
Untreated bunion pain progressively affects several key areas of daily function:
& Walking comfort — compensatory gait patterns develop, placing strain on the knees, hips, and lower back
& Footwear tolerance — the expanded joint prominence makes standard footwear increasingly difficult to wear without aggravating symptoms
& Joint integrity — ongoing malalignment accelerates cartilage wear within the first metatarsophalangeal joint
& Overall independence — reduced mobility impacts work capacity, physical activity, and general confidence
Addressing a painful foot prominence early, before structural joint damage is established, gives you the strongest chance of avoiding surgical intervention.
Protecting your mobility now is always preferable to managing a preventable complication later.
Book Your Bunion Assessment in Rosanna Today
For women in Rosanna living with daily bunion pain, taking the first step toward relief is often the most difficult part — but it doesn’t need to be. At Bellevue Podiatry, we offer a thorough bunion assessment that identifies the underlying causes of your pain and establishes a clear, conservative treatment pathway tailored to your needs.
You don’t need to choose between managing pain indefinitely or proceeding directly to surgery. Our approach centres on clinically appropriate, non-surgical options — including custom foot orthotics, targeted footwear modification, and ongoing personalised care designed around your daily routine and lifestyle demands.
Book your assessment at Bellevue Podiatry in Rosanna today. We’ll listen carefully, conduct a thorough clinical examination, and provide you with honest, evidence-based recommendations. Meaningful relief begins with a single appointment — and we’re ready to support you through every step of that process.
Frequently Asked Questions
How Long Does It Take for Custom Orthotics to Relieve Bunion Pain?
Custom orthotics typically begin to provide bunion pain relief within four to six weeks of consistent daily wear. This timeline reflects the gradual process of offloading pressure from the first metatarsophalangeal joint, allowing surrounding soft tissue inflammation to settle.
Most patients report meaningful comfort improvements by week eight, as the orthotic works to correct the biomechanical imbalances contributing to their symptoms. Consistency of wear during this period is clinically significant to achieving the best outcome.
Will My Bunion Get Worse if I Delay Treatment?
Yes, delaying bunion treatment can make your condition progressively worse over time. Without appropriate management, the first metatarsophalangeal joint continues to drift out of alignment, surrounding soft tissues become increasingly inflamed, and your pain intensifies with daily activity.
Early intervention using custom foot orthotics and footwear modifications has strong clinical evidence behind it for slowing the rate of progression. Addressing the underlying biomechanical drivers promptly helps preserve joint integrity and keeps you functional — reducing the likelihood of requiring surgical correction later on.
Are There Specific Shoe Brands Recommended for Women With Bunions?
Yes, certain shoe brands consistently perform well for women managing bunions. ECCO, Ziera, Naot, and Hoka are commonly recommended due to their wider toe boxes, deeper interiors, and supportive midsole structures that reduce pressure on the first metatarsophalangeal joint. New Balance and Brooks are also reliable options, particularly for walking and everyday use, as both brands offer generous width fittings suited to a broader forefoot.
That said, the brand itself is less important than achieving the correct fit for your specific foot shape. We always recommend pairing appropriate footwear with custom orthotics to address the underlying biomechanical contributors to bunion pain and slow its progression.
Can Bunion Pain Affect My Knees, Hips, or Lower Back?
Yes, bunion pain can absolutely affect your knees, hips, and lower back. Research indicates that up to 63% of people with bunions develop altered gait patterns, placing significant compensatory load on the entire kinetic chain — from the ankle through to the lumbar spine.
When you shift your weight or adjust your stride to avoid bunion pain, the resulting compensation disrupts normal joint mechanics at the knee, hip, and lower back. This cumulative stress, if left unaddressed, can accelerate wear on structures that were never designed to absorb that kind of irregular loading.
Early intervention is strongly recommended to prevent these secondary complications from developing or worsening over time.
Is Bunion Treatment Covered by Private Health Insurance in Australia?
Private health insurance can cover bunion treatment in Australia, depending on your level of extras cover.
Most funds contribute toward custom orthotics, podiatry consultations, and footwear modifications — the conservative treatments we specialise in at Bellevue Podiatry.
You will typically need a suitable extras policy that includes podiatry benefits.
Rebate amounts vary markedly between funds and individual policies, so we recommend confirming your entitlements directly with your insurer before commencing treatment.
Conclusion
Bunion pain doesn’t have to be something you simply endure or manage with the hope that surgery becomes your only option. At Bellevue Podiatry, locals from Rosanna, Heidelberg, Watsonia, Ivanhoe, and surrounding suburbs have access to evidence-based care grounded in extensive clinical research — giving you a clear, structured path toward lasting relief that addresses the root mechanics of your condition, not just the symptoms.
With personalised orthotics, targeted therapies, and expert footwear guidance, you can protect your mobility, reduce discomfort, and move through life with confidence again. The sooner you act, the more options you have — and the better your long-term outcomes are likely to be.