Persistent heel pain, plantar fasciitis, and tendon stiffness that fails to resolve with conservative measures such as rest, ice, and stretching are conditions we see regularly at our clinic. These presentations often indicate that the underlying tissue has entered a chronic, degenerative state rather than an acute inflammatory one, which is precisely why standard first-line treatments frequently provide limited relief.
Shockwave therapy works by delivering high-energy acoustic waves directly into the affected tissue, stimulating the body’s own healing response at a cellular level. This process promotes neovascularisation — the formation of new blood vessels — and encourages the breakdown of calcific deposits that contribute to ongoing pain. For patients in Rosanna and the surrounding areas who have plateaued with conventional care, this evidence-based treatment offers a clinically supported pathway toward meaningful, lasting recovery.
In This Article
- Shockwave therapy delivers acoustic energy pulses into damaged foot tissue to stimulate biological repair at the cellular level.
- Most patients experience measurable pain relief within two to three focused treatment sessions.
- It effectively treats stubborn conditions including plantar fasciitis, Achilles tendinopathy, and chronic heel pain unresponsive to conservative care.
- Treatment restores blood flow, stimulates collagen production, and breaks down calcific deposits without needles or injections.
- Shockwave therapy is available at Bellevue Podiatry and Rosanna Podiatry, serving patients across Rosanna and Heidelberg.
Why Rest and Ice Aren’t Curing Your Chronic Tendon Pain
If you’ve been icing your heel each night and resting for weeks, only to experience that same stabbing pain the moment you step out of bed, your body is signalling something important: passive treatments are no longer sufficient.
Chronic tendon conditions like plantar fasciitis fail to resolve with rest and ice alone because the tissue has entered a degenerative state, no longer capable of self-repair.
The affected area becomes increasingly deprived of blood flow, trapping the tissue in a cycle of persistent pain and stalled recovery.
Extracorporeal shockwave therapy (ESWT) is a clinically supported treatment that addresses this directly, stimulating cellular repair at the level of the plantar fascia rather than simply masking symptoms.
It isn’t a temporary measure — it’s a targeted intervention designed to restart the healing process where passive care has failed.
What Is Shockwave Therapy and How Does It Work?
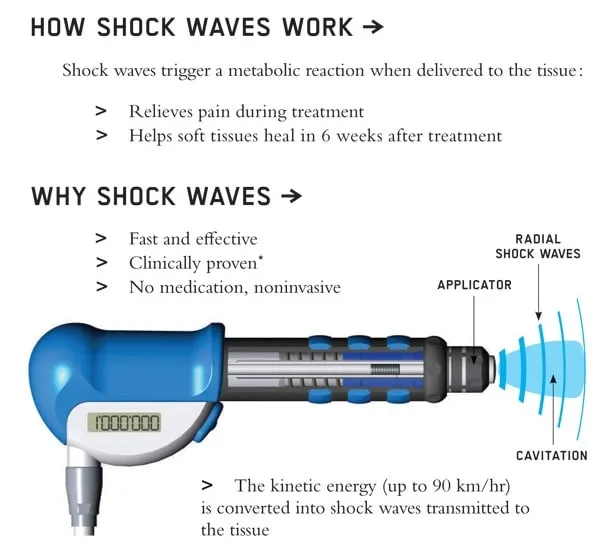
Shockwave therapy delivers focused acoustic energy pulses directly into damaged soft tissue, stimulating a series of biological responses that support the body’s natural healing process. It’s a clinically validated, non-invasive treatment used widely in podiatric practice for persistent musculoskeletal conditions.
The treatment works by penetrating the affected tendon or fascia at a cellular level, where it promotes increased blood flow, breaks down calcific deposits, and stimulates collagen production to support tissue repair. There are two primary delivery methods used clinically:
- Focused shockwave therapy – directs concentrated energy to a precise, targeted point within the tissue
- Radial shockwave therapy – disperses energy outward from the treatment head, covering a broader injury zone
Top Lower Limb Conditions Treated with Shockwave
Shockwave therapy isn’t a one-trick solution — it’s a clinically proven tool that targets several of the most stubborn lower limb conditions that defeat conventional treatment.
Whether you’re battling the searing morning heel pain of plantar fasciitis, the chronic Achilles tendon damage that won’t let you run, or the relentless shin splints that sideline your training, shockwave delivers targeted acoustic energy precisely where your body has stopped healing.
Here’s a closer look at the three conditions our Rosanna patients most commonly bring to us — and why shockwave is changing their outcomes.
Plantar Fasciitis and Severe Heel Pain
Plantar fasciitis is one of the most common — and most undertreated — musculoskeletal conditions we manage at Bellevue Podiatry. If you have already trialled rest, orthotics, and stretching without sustained relief, shockwave therapy may be the next appropriate step in your care.
Our approach to chronic heel spur treatment is focused on addressing the underlying pathology, not simply managing symptoms. For patients with persistent plantar fasciitis, shockwave therapy offers a clinically supported mechanism for genuine tissue recovery.
Shockwave therapy works by delivering targeted acoustic energy to the affected area, producing the following therapeutic effects:
- Breaking down calcified deposits within the fascia and around the heel
- Stimulating collagen production to support the repair of damaged connective tissue
- Restoring localised blood flow to degenerative, poorly perfused tissue
- Reducing nerve sensitivity responsible for the characteristic stabbing pain experienced during those first steps in the morning
If conservative management hasn’t provided lasting improvement, this treatment warrants serious consideration as part of your ongoing care plan.
Achilles Tendonitis and Ankle Issues
Achilles tendonitis is a particularly stubborn condition that responds well to shockwave therapy (ESWT), especially when months of stretching, load management, and physiotherapy haven’t restored full function.
In chronic cases, the tendon tissue often becomes degenerative rather than simply inflamed — a state known as Achilles tendinopathy — which means conventional approaches are unlikely to stimulate the deep cellular repair needed for meaningful recovery.
At Bellevue Podiatry, we use Extracorporeal Shockwave Therapy (ESWT) as a clinically recognised, evidence-based option for tendon regeneration.
The treatment works by delivering targeted acoustic energy directly into the tendon, breaking down calcific deposits, promoting growth factor release, and stimulating stalled collagen production.
Whether your pain is mid-portion or insertional, ESWT offers a structured, non-surgical pathway to restoring tendon function with minimal downtime.
Shin Splints and Running Injuries
Runners dealing with persistent shin splints often find that rest and foam rolling provide only temporary relief, because these approaches don’t address the underlying periosteal inflammation driving the condition. Shockwave therapy is a clinically supported treatment that targets chronic tissue dysfunction at its source, promoting genuine healing rather than symptom management.
At Bellevue Podiatry in Rosanna, we apply shockwave therapy directly to the stress points responsible for your pain, using controlled acoustic waves to stimulate the body’s own repair mechanisms where they’ve stalled.
Shockwave therapy addresses the key physiological factors that sustain running injuries:
- Periosteal inflammation — desensitises overloaded bone membrane pain signals at the site of injury
- Microtear accumulation — stimulates collagen synthesis to rebuild compromised soft tissue structures
- Poor localised circulation — promotes angiogenesis, restoring blood flow to under-perfused tissue
- Recurring injury cycles — corrects underlying tissue dysfunction rather than masking symptoms
For runners experiencing repeated setbacks with shin splints, shockwave therapy offers a pathway to durable recovery and a safe return to training.
The Real Benefits of Investing in Shockwave Treatment
When you choose shockwave therapy, you’re not masking your pain with needles or numbing agents — you’re triggering your body’s own repair mechanisms at the cellular level.
The focused acoustic energy stimulates blood flow, breaks down dysfunctional tissue, and jumpstarts collagen production in tendons that have stubbornly refused to heal on their own.
Most patients experience measurable pain relief within just a few sessions, making this one of the fastest-acting non-surgical solutions available for chronic foot and heel conditions.
Fast-Acting Pain Relief Without Injections
Many patients notice a meaningful shift in their pain levels within the first two to three sessions of shockwave therapy — a response rate that makes it one of the more clinically effective options we offer for chronic foot pain.
Unlike cortisone injections, which suppress inflammation chemically and often provide only short-term relief, shockwave therapy works by stimulating the body’s own repair mechanisms at the tissue level. This distinction matters when we’re managing conditions that involve genuine structural or degenerative damage.
The key clinical advantages include:
- No needles or pharmacological agents — healing is stimulated biochemically through targeted acoustic energy
- Rapid reduction in localised inflammation — by disrupting aberrant pain signalling at the affected tissue
- Cumulative therapeutic benefit — each session reinforces the last, supporting progressive tissue repair
- Sustained outcomes — by addressing the underlying pathology rather than masking the presenting symptoms
What this means for you as a patient is that we’re not simply managing your discomfort in the short term. We’re working to restore the tissue integrity that cortisone alone can’t reliably achieve over time.
Accelerating the Body’s Natural Healing Process
What makes shockwave therapy clinically valuable isn’t simply faster pain relief — it actively restarts a healing process that has stalled in chronically affected tissue. At Bellevue Podiatry, we’ve seen this technology resolve cases where months of conservative management, including rest and physiotherapy, produced little to no improvement.
| What Shockwave Targets | What Your Body Does |
|---|---|
| Dormant, degenerated tissue | Rebuilds collagen fibres |
| Calcific tendinitis treatment sites | Dissolves calcium deposits |
| Restricted blood supply | Stimulates new vessel growth |
Each session delivers acoustic waves deep into damaged structures, triggering genuine biological repair at a cellular level. For chronic presentations, this is not symptomatic masking — it is a measurable physiological response that supports long-term tissue recovery.
What to Expect During Your Rosanna Podiatry Session
Stepping into your shockwave therapy session at Bellevue Podiatry, you can expect a structured, clinically guided process from start to finish. Our approach is precise, evidence-based, and tailored to the specific injury presentation each patient brings through the door.
Precise, evidence-based, and tailored — every shockwave therapy session at Bellevue Podiatry is structured around your specific injury.
Here is what your session involves:
- Assessment — Your podiatrist identifies the exact injury site through clinical examination, ensuring treatment is accurately targeted.
- Gel application — A conductive gel is applied to the skin to optimise acoustic wave transmission to the affected tissue.
- Treatment delivery — Controlled pulses are delivered over 5–10 minutes, stimulating localised blood flow and initiating breakdown of damaged tissue.
- Immediate aftercare advice — You’ll leave with clear, practical guidance on activity modification and what to expect during recovery.
We treat patients across the Rosanna and Heidelberg areas, and every session is kept focused, efficient, and aligned with your recovery goals.
Frequently Asked Questions
How Many Shockwave Therapy Sessions Will I Need to See Results?
Most patients require between 3 to 6 shockwave therapy sessions to achieve meaningful clinical results, with each treatment spaced approximately one week apart.
Some patients notice a reduction in pain after the first or second session, though genuine tissue repair and regeneration occurs progressively over the full course of treatment.
Your podiatrist will tailor the number of sessions to your specific diagnosis, symptom severity, and how your body responds to each treatment.
Chronic conditions such as plantar fasciitis or Achilles tendinopathy typically require the complete recommended course to achieve lasting, measurable improvement.
Is Shockwave Therapy Painful, and What Does It Feel Like?
Shockwave therapy is generally described as uncomfortable rather than painful.
Most patients report an intense pulsing or tapping sensation directly over the treated area, often accompanied by mild aching or tenderness — particularly over inflamed soft tissue or bony insertions.
Sensitivity during treatment is normal and typically settles within the first minute as your body adjusts to the stimulus.
If discomfort becomes sharp or difficult to tolerate, the intensity can be modified to suit your threshold without compromising clinical outcomes.
Does Private Health Insurance Cover Shockwave Therapy in Rosanna?
Coverage for shockwave therapy under private health insurance in Australia varies depending on your individual policy and fund. Most insurers currently classify it as an emerging treatment, meaning it may not attract a direct rebate under its own item number.
However, if your extras cover includes physiotherapy or podiatry consultations, you may receive partial reimbursement through those categories.
We recommend contacting your insurer directly before your appointment to confirm what rebates apply to your specific policy. Our team at Bellevue Podiatry can also assist by providing the appropriate treatment codes to support your claim.
Are There Any Contraindications That Would Prevent Me From Receiving Shockwave?
Yes, there are a few contraindications that would prevent shockwave therapy from being a suitable option. These include pregnancy, blood clotting disorders, active infection, or the presence of malignancy near the treatment site.
If you have received a corticosteroid injection in the affected area within the past 12 weeks, a waiting period is also required before proceeding.
Your podiatrist will conduct a thorough review of your full medical history during your initial consultation to confirm you’re a safe and appropriate candidate for treatment.
How Soon After Shockwave Therapy Can I Return to Sport?
Most patients can return to low-impact activity within 24–48 hours following shockwave therapy.
High-impact sport, however, should be avoided for 3–5 days post-treatment, as the targeted tissues are actively undergoing biological remodelling during this window.
Returning to load too early can disrupt the healing cascade that shockwave therapy initiates, potentially reducing its effectiveness.
Your podiatrist will provide a personalised return-to-sport timeline based on your condition’s severity, your individual treatment response, and the specific physical demands of your sport.
Conclusion
If months of conservative treatment have left you no closer to pain-free mornings, shockwave therapy offers a genuine path forward. At Bellevue Podiatry, our evidence-based approach — grounded in extensive clinical research — is designed to restart your body’s natural healing process where other treatments have stalled. We proudly support locals from Rosanna, Heidelberg, Watsonia, Ivanhoe, and the surrounding suburbs, bringing proven podiatric care closer to home.
Your tendons deserve more than another round of rest and hope. With the right intervention, lasting relief is well within reach — and it starts with taking that first step.